For more references to the literature on various aspects of the dental bite, or dental occlusion – there is a good section in Wikipedia covering this topic.
Organization of this Chapter
The Basics
How the Teeth Fit Together
How the Teeth Slide Over each Other
How the Joints Direct Closure
Bottom line for the Bite
…………………………………………………………………………………………………………………………
The Basics
Consider that you have just eaten something will little tiny seeds! Maybe a fig or something else that may be a personal favorite. Have you discovered that when just ONE little seed gets stuck on the surface of one tooth, the opposing tooth doesn’t bite down completely, and the entire BITE is off? You may have marveled, perhaps subconsciously, that such a small thing can have such a large impact on your comfort.
Besides the fact that very small deviations can alter the bite in a very noticeable way, there are other things that make the study of the bite challenging. One of the difficulties with the gathering of evidence to test theories of bite irregularities and the harm they can cause is that the progression of the disorders occurs over a long time period, often years or decades. Another problem is that the disorders of the mouth are most certainly caused or aggravated by many factors, the bite being just one.
Nonetheless, it is clear that the accuracy of the bite is very important for maintenance of a healthy mouth. We shall, then, in the present chapter describe the ideal bite characteristics, and in later Chapters discuss the relationship between non-ideality and dysfunction and potential for correction.
Visit Chapter III.4 for a discussion of grinding. Visit Chapter V.15 for a discussion of the collapsed bite and full mouth rehabilitation.
First, however, we must define another term, OCCLUSION. This term is used quite often in dentistry, for it relates to many considerations of how the teeth bite together. The biting surface of each tooth is the OCCLUSAL SURFACE. The plane of the teeth in each arch (not a flat plane, by the way) is referred to as the occlusal plane. And all details of the way the teeth come together and move over each other as the chin is shifted side-to-side or forward are lumped together in the study of DENTAL OCCLUSION. A more proper term that is used by gnathologists is stomatognathics, but we’ll stick to “occlusion”, or even simpler, the BITE. Also, when the teeth are touching as the mouth is closed, they are said to be IN OCCLUSION.
Even most dentists don’t have a thorough understanding of occlusion. The subject is taught in dental schools, but is not thoroughly studied except by students who elect to do graduate studies in a prosthodontic specialty, or by general dentists who study independently with the few great clinicians and teachers in the field. I was incredibly lucky when I was a dental student to be able to study with Dr. Robert Lee, one of the most experienced educators and clinicians in full mouth rehabilitation ever to enter the field. He taught classes privately in the town next door to my dental school. What I learned is that the occlusion is a subject worth a lifetime of study!
The Dental Bite: How the Teeth Fit Together
With a normal complement of 28 teeth, assuming the wisdom teeth have been removed, the number of separate points of contact between the upper and lower teeth when biting down may be 80 – yes EIGHTY! This is the ideal situation where the teeth fit together exactly as DESIGNED. Each of the cusps of a posterior tooth fits into a fossa of the opposing tooth such that it is stabilized by three points of contact, arranged in a nearly equilateral triangle. As indicated earlier, unless the teeth are stabilized against movement they will move, and it is clear that the interlocking of the teeth in occlusion is a very stable condition.
Note the way the teeth in the following picture fit precisely together, and we can’t even see the details of the biting, occlusal, surfaces.
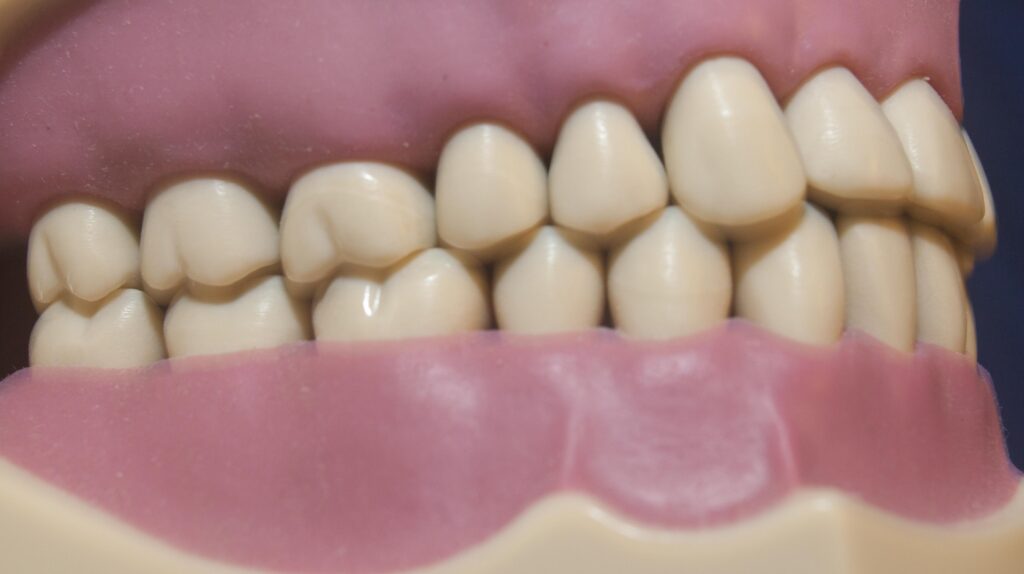
You might ask yourself if the dentist, when placing a filling or crown (that replaces parts of the tooth that were in contact) can rebuild the contacts exactly the way they were originally. The answer is yes, if enough effort is expended. Unfortunately, in the general practice of dentistry, the occlusal contacts are seldom established with great precision. Possible consequences of this situation will be discussed later, but first let us look more closely at nature’s ideal plan.

The picture below shows the contact points on one half of the mouth, where both the upper and lower teeth touch. The dark spots which indicate ideal contact points show the triangular arrangements that stabilize opposing cusps. It seems truly phenomenal that such an arrangement was planned genetically and that the execution of this plan is carried out by cells that migrate from the nervous system in the fetus to specific locations in the mouth to form teeth of exactly specified shape, which when they erupt will all fit together with such utter perfection! In fact, this plan in real life falls in the category of “best laid plans”. It is the rare individual that has such perfect occlusion!
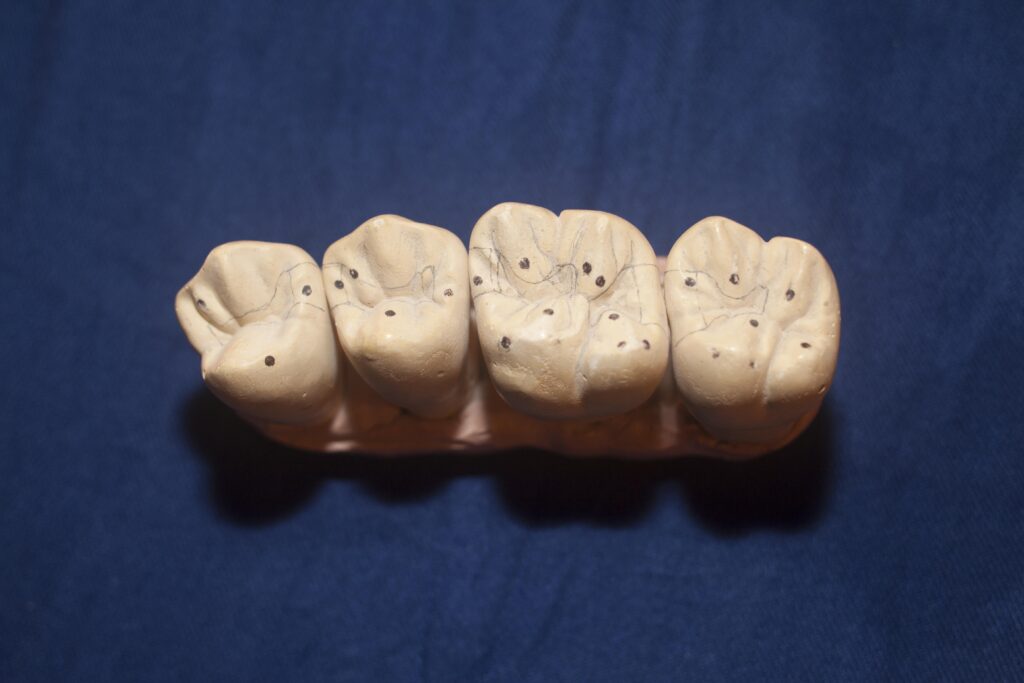
We will discuss later what causes deviation from ideal occlusion, and then what problems these deviations can cause, and what can be done about it. Visit Chapter V.17 for a discussion of orthodontics. But first, we will continue our look at the design itself. When the dentist takes on the task of rebuilding someone’s dentition, it is necessary to have a good concept of the target, and the target should be to fit the teeth together as they were designed.
Before looking at the MOVEMENTS of the teeth relative to each other, we must first define two new terms. When a person bites so that the teeth fit together as well as possible, such that they are in their most stable interlocking position, this is called CENTRIC OCCLUSION, or a newer term is MAXIMUM INTERCUSPAL POSITION, MIP. It defines a relationship between the teeth, but it does not describe how the teeth would come together as the jaw naturally hinges with the joint rotating in the most comfortable position. If the joint is fully seated and the mouth closed, the teeth SHOULD come together in centric occlusion, but often will not. The teeth may come together so that one cusp will hit another. How the teeth come together when the JOINT is seated has traditionally been called CENTRIC RELATION, and centric relation is not necessarily the same as centric occlusion although it ideally would be.
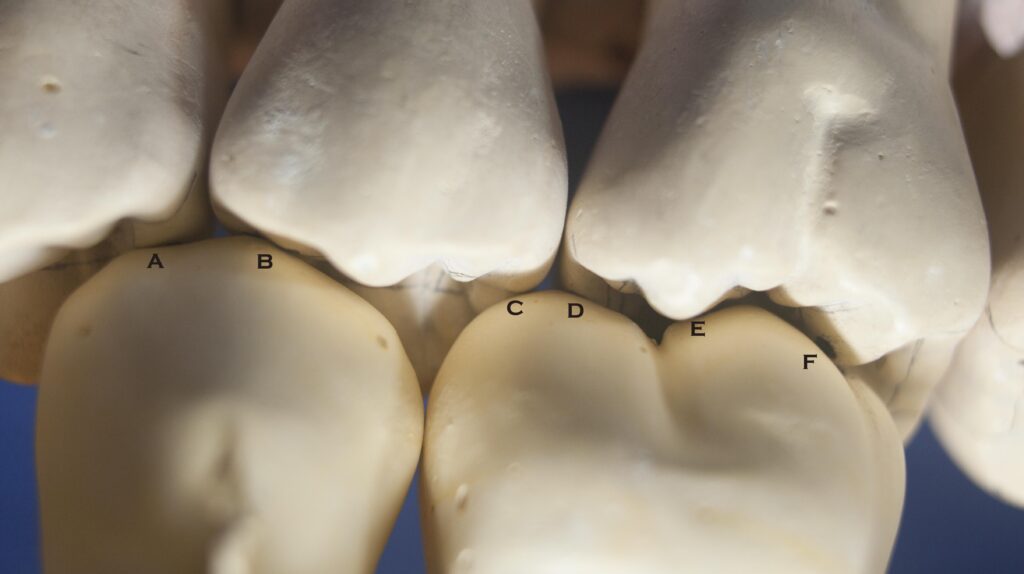
Later we will look in more detail at discrepancies between centric occlusion and relation and see if such a discrepancy could cause problems. Visit Chapter V.15 for a discussion of full mouth reconstruction – which depends on understanding a particular patient’s jaw movements in relation to their bite very well.
The Dental Bite: How the Teeth Slide Over each Other
Having some understanding of the ideal occlusion leads us to an examination of movements of the teeth away from this position. Chewing patterns require that the upper and lower teeth move in a complex fashion relative to each other. It is the ideal situation that as one cusp leaves its occlusal contact position it moves along grooves in the surface of the opposing partner. Chewing has a component of its motion that takes cusps through opposing grooves, in this way the crushed food can be swept off the surface of the tooth and room made for more. It is a side-to-side motion that causes this to happen.
But chewing is not the only activity that moves the teeth over each other. Swallowing causes the teeth to come together. If your centric relation and occlusion positions are different, your hinging motion would not take you to ideal closure and thus a correction must be made at the last instant. This correction may cause a slide of the teeth – this is non-ideal and its direction would not necessarily correspond to a natural feature like a groove. Also, if you bite down in this case it might force the condyle OUT of the fossa, which can result ultimately in trauma to the disc.
Another activity that moves the teeth relative to each other is unconscious function. In this case you simply slide your teeth to different positions, either side-to-side or by moving your chin forward, or a combination of both, without being aware of it. If you exert substantial pressure in these movements then damage can result, and a section will be devoted to that subject later. Visit Chapter III.4 for a discussion of tooth grinding.
No matter what tends to move the lower teeth side-to-side or forward relative to the uppers, there is a particular design aspect of the occlusion that helps to protect the teeth from damage. This natural feature is called DISCLUSION. You can test to see if your teeth have adequate disclusion. With your teeth always in contact, slide your jaw either to the right or left. When you do this the only teeth that should be touching are the right or left CANINES. These particular teeth seem to have been designed to take the load of lateral excursions and not allow the posterior teeth to touch except in a position very close to centric occlusion.
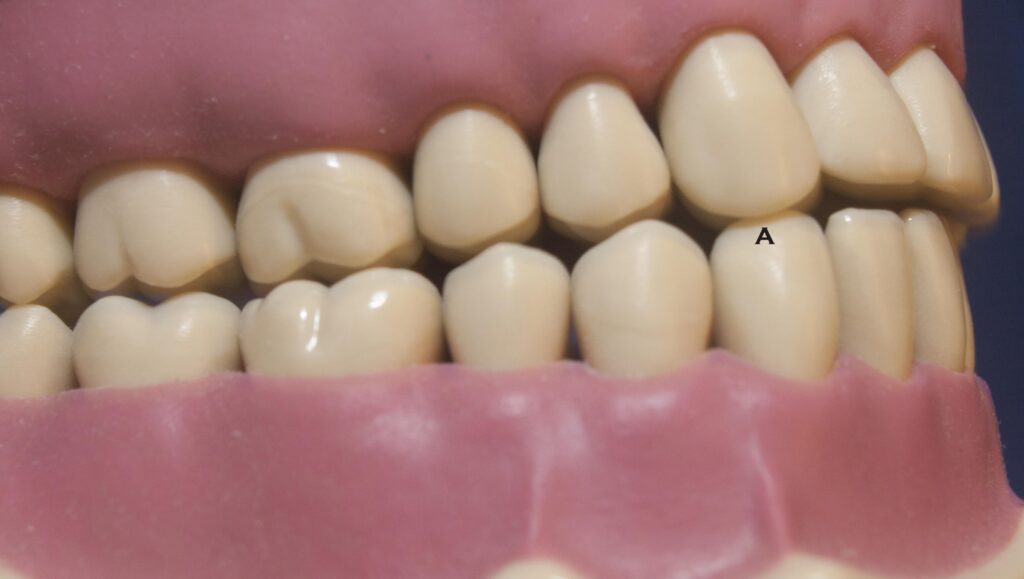
Try moving your lower teeth forward while touching your upper incisors. Did you feel the posterior teeth touch? If so, then you have inadequate anterior guidance in this movement. The guidance offered by the anterior teeth so that the posterior teeth do not touch in these excursions is called, appropriately enough, anterior guidance. The anterior guidance is generally good if you have adequate overbite in the front. Overbite is the amount of vertical overlap that exists as the upper teeth extend down over the lower incisors when you bite together. With ample overbite, AND (as we saw in the last section) a relatively steep slope in the joint socket, the posterior teeth must separate in lateral or forward movement.
Why is it important that the posterior teeth separate? One needs to think about what happens if they don’t. When the anterior teeth are ground flat due to strong excursive habits, then the posterior teeth can start grinding on each other. This causes tooth breakdown in a variety of ways. If you do not tend to grind your teeth as a bad habit, but have poor anterior guidance due to tooth malposition, then your normal chewing patterns will not be guided in closure by the anterior, particularly the canines. This means that there will be inaccurate closures during chewing which can tend to slide cusps over each other and lead to wear or other traumatic damage.
With a typical amount of anterior overbite, when the jaw is moved forward, into protrusion, it is often the case that the canines cause the incisors to separate. This protects the incisal edges of these teeth. The value of this is particularly important when the anterior teeth are restored by porcelain crowns, which are very abrasive. If the canines do not disclude the incisors in protrusion, the incisors can be ground down so far that they are half gone!
The Dental Bite: How the Joints Direct Closure
As we discussed earlier, centric relation describes the relative positions of the upper and lower teeth as the jaw hinges closed with the joint fully seated. What determines whether your joint is fully seated when your jaw closes? To a large extent it may be whether your teeth come together well in this position! This is starting to sound like the cart got before the horse, or the egg laid the chicken ….
The important thing to note is that theories of occlusion and jaw closure are not typically universally accepted. Again, we are in an area that is fiendishly difficult to prove by objective standards. There are practitioners that have studied the area for 30 years and have operated using a set of concepts based on a particular theory and have had a very high success rate. Other practitioners have used different approaches and claim great success as well. How well documented are their claims? This is often difficult to judge. The bottom line is, however, what makes sense to the dentist, as long as it provides good service to the patients.
It is clear that the brain directs closure of the jaw. There is strong unconscious control of the jaw movement, and this can easily be demonstrated in many individuals by having a friend attempt to hinge your jaw up and down while you relax your muscles. If you are typical, you will not be able to let him move your jaw freely no matter how hard you try. This is because your brain doesn’t want him to bang your teeth together, for fear that some damage will result. Likewise, it makes sense that if closure with your joint seated would cause your teeth to hit each other, the muscles will pull the joint out of place in order to adjust the position of bite to be more comfortable.
It doesn’t happen often, but do you remember a time when you were eating or talking or doing something when all of a sudden your teeth hit together and it really jarred your head? It is quite shocking when it happens, and you can readily understand why the brain would like to avoid it if possible. Of course, if your centric relation position and your centric occlusion position are coincident, this is less likely to happen. If you have adequate anterior guidance, this CANNOT happen.
Now we have looked enough at the joint and bite to understand most of the concepts that come into play with whole mouth problems in dentistry. As indicated before, the theories are not necessarily unanimously accepted, but it is only important that you are aware of the issues. This knowledge will be sufficient when we discuss the breakdown of ideality and the advent of disease and dysfunction.
Bottom Line for the Dental Bite
For many people it is the dental BITE that is the most troubling thing about their mouth. If the bite is “off”, where you might bite down on one side of the arch differently from biting on the other side, it can disturb your sense of comfort and balance. This may be subtle, or it may lead to clenching, muscle fatigue, trauma to teeth and pain. When the bite is not comfortable some people attempt to grind down the teeth so they fit together better – of course this is subconscious. On the other hand, some people grind their teeth together out of emotional stress, and that creates disharmonies in the bite pattern which, potentially, creates more stress.
The bite, or occlusion, is a complex, and multifactorial subject. It is worthy of careful consideration by patient and clinician alike, if there is any chance of increasing the comfort level of the patient.